Assessment in the Acute care Setting
When an older person comes into acute care, a whole range of data must be collected in a standardised and comprehensive way. For this reason, an assessment tool is usually used. Illnesses in older people can be misdiagnosed, overlooked or mistaken as normal ageing processes, especially when health professionals don't recognise the ways that diseases and drugs can affect older patients. A thorough admission assessment can help ensure that assessment is accurate and useful. However, it is important to realise that assessment is not a one-off activity, but an ongoing and dynamic process. The health status of older patients can often change several times during one admission.
To assess older people in the acute setting, just generally you really need to know something about the facility you are working in because most facilities would have a tool that would help you document your assessment and will provide you some guidelines how to go about the process.
When you are working with the older people what you need to remember is that older peoples aging impacts on their health in general, so they will have a whole range of issues that you need to look at, not just one or two aspects and that in the assessment process it will take them some time to answer you because they tend to answer a bit slower, think a bit slower. So you need to actually allow more time and you also need to gather more information. The documentation tool can help you with that, help you to guide the process and guide your thinking about what you need to assess.
When you assess an older person it’s very important that we also take into consideration other people, for example, the person who brings them in can very often give you some valuable information, particularly when your caring for an older person who is that confused because they are unwell and they may not remember the information that you want to have or they may not be able to give it to you clearly. In that case it can be very valuable to talk to other people who can give you background information. They can also very often tell you about medication the person is taking and even bring it in if you ask them to, which makes it very good.
The other thing is that we can gain enormous amount of information from patients just by observing what they do while they are for example, having their meals, having their showers, dressing and undressing. You can see things like range of moment in the joints, you can see how much they eat, how well they eat, whether they pick a wide variety of food. So without needing to ask them you can as often get significant information just by observing what they are doing.
When you have a confused person it’s even more important that you do it slowly because they need some time to get use to you and to get use to the environment before you actually start doing your assessment. If you start too early and they are confused and frightened, they may not give you an accurate picture of what’s really happening health wise.
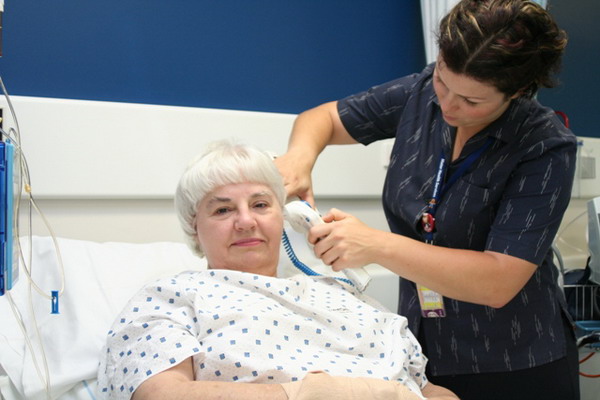
Jenneke talks in the video about taking time to conduct an initial assessment of an older client. She also mentions other ways of gathering information such as talking to carers and observing the client engaging in activities such as showering and eating meals.
How might you integrate the collection of assessment data into other care activities?
Thinking challenge
Holistic and comprehensive assessment and care of all clients is important, but can be even more important, complex and involved with older clients. After investigating the link below, consider the following questions:
- What do you imagine some of the consequences might be if the older acute care patient is not assessed and treated comprehensively?
- How might this have an impact on your understanding of the client?
- What impact might it have on the effectiveness of their healthcare?




